
become increasingly prevalent. Despite various randomized trials, the
most adequate fixation technique of fragility fractures has not yet been
identified [79]. Available fixation techniques include Kirschner wire
fixation, intrafocal pinning using the Kapandji technique, external
fixation with bridging fixators, and internal fixation using dorsal or
volar plates [80]. Bone grafts and calcium phosphate cements have
been utilized singularly or in combination with other fixation
techniques in order to augment them. When operative treatment is
indicated, the volar locking plate osteosynthesis has become the
treatment of choice [81]. Anatomically pre-contoured volar locking
plates are most commonly used. If correctly applied they allow for early
motion and have an acceptable complication profile [40,78,82]. The
development of locking compression plates offered the possibility of
volar plate fixation for those fractures with dorsal angulation and
comminution. The volar approach minimizes soft-tissue problems
while the angle stable screws maintain radial length without the
need for a buttress [41]. In order to improve the development of volar
locking compression plate osteosynthesis recent cadaveric studies
demonstrated that cement augmentation improves biomechanical
performance of volar plating of the distal radius [83] in order to avoid
implant failure due to secondary loss of reduction and articular screw
perforation (Figure 2).
Fragility fractures of the femur
Fractures around the hip have a high morbidity and mortality in
the elderly population with up to 30% of patients dying within
one year after surgery [84]. Proximal femoral fractures in the
elderly are still increasing and are frequently associated with
osteoporosis [85]. Intracapsular, undisplaced or impacted fractures
are normally managed by internal fixation using modern angle
stable multiple screw fixation systems (Figure 3) [48] or a dynamic
hip screw (DHS). Although a major technical problem is secondary
fracture impaction, the DHS allows this to occur along the axis of
its screw. Accurate placement of the screw in the femoral head is
best measured by the tip-apex distance and affects the performance
of the device.
Particularly in osteoporotic bone the management of displaced
extracapsular fractures is more controversial. The basic surgeons
’
choice is between prosthetic replacement, or open reduction and
internal fixation. In general, age is not important but biological age
with pre-injury mobility, residential status and cognitive function
affect prognosis and are key factors for decision making. AO type 31 A1
and A2 fractures can be fixed by extramedullary as well as
intramedullary osteosynthesis with no generalizable advantage for
one or the other technique [86]. Unstable trochanteric and sub-
trochanteric fractures
–
especially AO/OTA type 31 A3 fractures
–
require open reduction and internal fixation. Although convincing
clinical evidence still needs to be provided, it appears that cephalo-
medullary nails are preferable over extramedullary devices for these
unstable fracture types [53,87]. Nevertheless, cephalomedullary
nailing systems combine the biomechanical advantages of a sliding
hip screw with those of intramedullary nailing. The sliding hip screw
provides a controlled impaction of the fracture, leading to increased
fracture stability, less collapse and decreased bone healing time. The
intramedullary nail is located closer to the central weight bearing axis
of the femur and thus reduces bending stresses by up to 30% due to
shorter lever arm [88]. Mechanical implant breakage is a rare but
relevant complication of cephalomedullary nailing systems especially
in subtrochanteric or malreduced fractures with varus axis deviation of
the proximal fragment, and is often a consequence of nonunion due to
the effect of adverse shear forces [89,90].
Finally, in osteoporotic fractures of the distal femur, good
radiological and functional results have been reported for the
application of the anatomical angle stable plate osteosynthesis [91]
but also with other angle stable fixation techniques [92].
Fragility fractures in the spine
Vertebral fractures in the elderly population constitute two
different entities: traumatic fractures in osteoporotic bone and fragility
fractures without adequate trauma. Vertebral fragility fractures are
associated with relevant deterioration of vertebral biomechanical
properties leading to the occurrence of subtle and often non-
symptomatic wedge fracture. Indications for surgical intervention in
osteoporotic patients are similar to non-osteoporotic patients and
include radiculopathy, myelopathy, back pain, progressive spinal
deformity with or without fracture, neurogenic claudication, and
failure of conservative management [93]. Several surgical techniques
have been developed to treat osteoporosis-related deformities,
including posterior instrumentation with fusion [94]. Augmentation
methods to improve pedicle screw fixation have evolved [95], including
instrumentation at multiple levels, bioactive cement augmentation,
and fenestrated or expandable pedicle screws, but their impact on
clinical outcomes remains unknown.
Early mobilization is the key for improved outcome of patients with
thoracolumbar fragility fractures. Surgical stabilization, including the
use of bone cement, may be helpful in achieving this goal, although
there is ongoing debate on the efficacy of this approach [96]. Options
Fig. 2.
Post mortem verified implant failure of an angle stable volar plate fixation in
an osteoporotic distal radius AO/OTA type C fracture. Collapse of the fracture and
articular perforation of the screws.
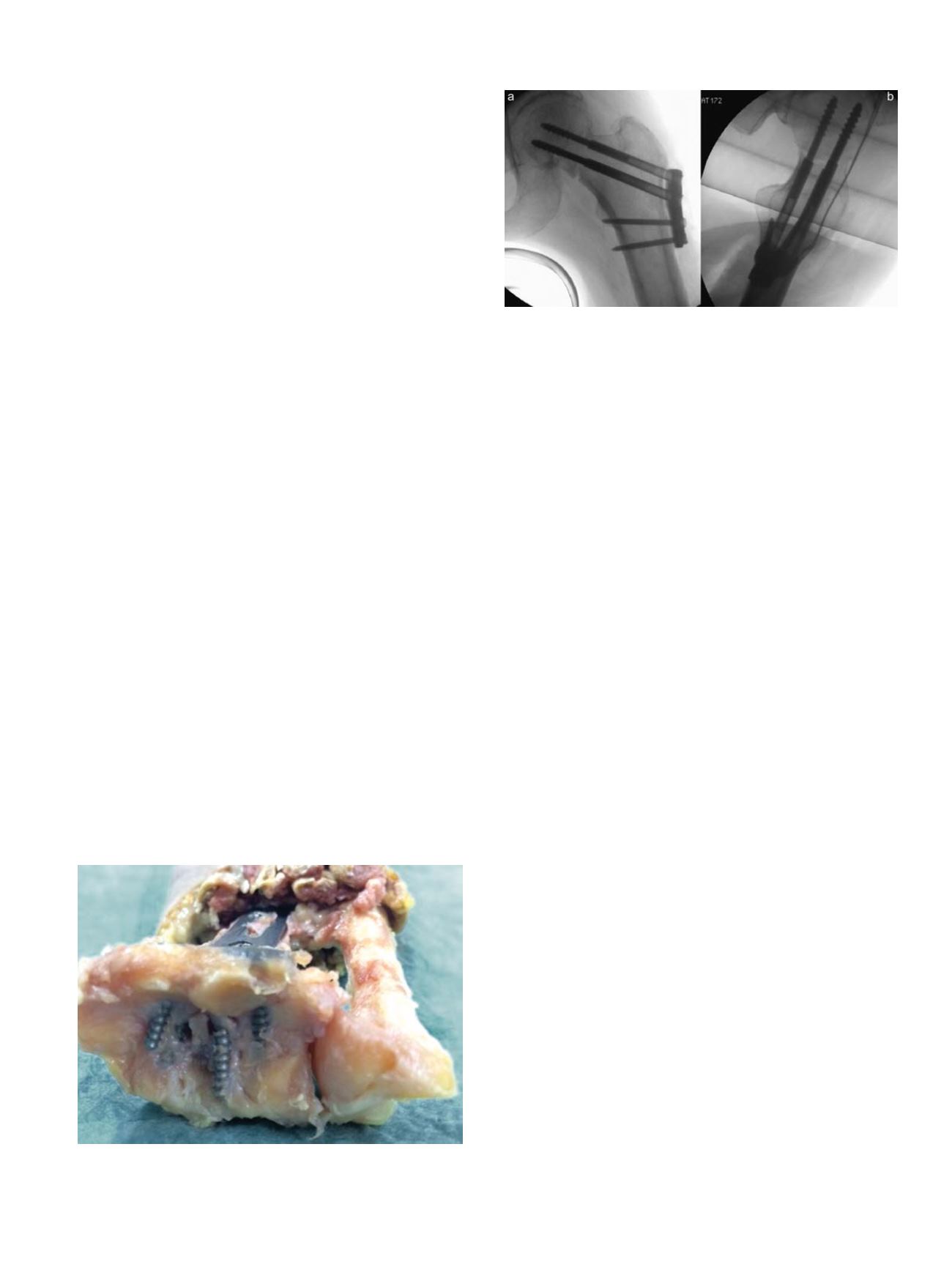
Fig. 3.
Fixation of a Pauwels type III fracture of the femoral neck with a pin and plate
construct (Targon, Aesculap). The plate provides angle stable support for the pins, an
increased area of load support, while the screws can still slide and compact the frac-
ture. (a: anterior-posterior and b: axial view).
C. von Rüden, P. Augat / Injury, Int. J. Care Injured 47S2 (2016) S3
–
S10
S7


















