
Conflict of interest
The authors have no conflicts of interest.
Acknowledgment
The study was sponsored by a travel grant from Germany/Hong Kong
Joint Research Scheme (Ref: G_HK009/07) of the German Academic
Research Service (Deutscher Akademischer Austauschdienst (DAAD))
funded by means of the Federal Ministry of Education and Reserach of
Germany (Bundesministeriums für Bildung und Forschung (BMBF)).
The authors thank aap Biomaterials, Dieburg, Germany, for the
provision of the OSTIM
®
and OSTIM
®
+ collagen type-I implants.
References
[1]
Van Lieshout EM, Alt V. Bone graft substitutes and bone morphogenetic proteins for
osteoporotic fractures: what is the evidence? Injury 2016;47(Suppl 1):S43
–
6.
[2]
Canuto RA, Pol R, Martinasso G, Muzio G, Gallesio G, Mozzati M. Hydroxyapatite paste
Ostim(®), without elevation of full-thickness flaps, improves alveolar healing stimulating
BMP- and VEGF-mediated signal pathways: an experimental study in humans. Clin Oral
Implants Res 2013;24(Suppl A100):42
–
8.
[3]
Zaffe D, Traversa G, Mozzati M, Morelli F, D
’
Angeli G. Behavior of aqueous
nanocrystalline hydroxyapatite in oral bone regeneration. J Appl Biomater Biomech
2011;9:19
–
25.
[4]
Huber FX, McArthur N, Heimann L, Dingeldein E, Cavey H, Palazzi X, et al. Evaluation of a
novel nanocrystalline hydroxyapatite paste Ostim in comparison to Alpha-BSM - more
bone ingrowth inside the implanted material with Ostim compared to Alpha BSM. BMC
Musculoskelet Disord 2009;10:164.
[5]
Huber FX, Hillmeier J, Kock HJ, McArthur N, Huber C, DiwoM, et al. [Filling of metaphyseal
defects with nanocrystalline hydroxyapatite (Ostim) for fractures of the radius]. Zentralbl
Chir 2008;133:577
–
81.
[6]
Thorwarth M, Schultze-Mosgau S, Kessler P, Wiltfang J, Schlegel KA. Bone regeneration in
osseous defects using a resorbable nanoparticular hydroxyapatite. J Oral Maxillofac Surg
2005;63:1626
–
33.
[7]
Spies CK, Schnürer S, Gotterbarm T, Breusch S. The efficacy of Biobon and Ostim
within metaphyseal defects using the Göttinger Minipig. Arch Orthop Trauma Surg
2009;129:979
–
88.
[8]
Brandt J, Henning S, Michler G, Hein W, Bernstein A, Schulz M. Nanocrystalline
hydroxyapatite for bone repair: an animal study. J Mater Sci Mater Med 2010;21:283
–
94.
[9]
Chris Arts JJ, Verdonschot N, Schreurs BW, Buma P. The use of a bioresorbable nano-
crystalline hydroxyapatite paste in acetabular bone impaction grafting. Biomaterials
2006;27:1110
–
8.
[10]
Busenlechner D, Tangl S, Mair B, Fugger G, Gruber R, Redl H, Watzek G. Simultaneous in
vivo comparison of bone substitutes in a guided bone regeneration model. Biomaterials
2008;29:3195
–
200.
[11]
Di Lullo GA, Sweeney SM, Körkkö J, Ala-Kokko L, San Antonio JD. Mapping the ligand-
binding sites and disease-associated mutations on the most abundant protein in the
human, type I collagen. J Biol Chem 2002;277:4223
–
31.
[12]
Gelse K, Pöschl E, Aigner T. Collagens
—
structure, function, and biosynthesis. Adv Drug
Deliv Rev 2003;55:1531
–
46.
[13]
Pierschbacher MD, Ruoslahti E. Cell attachment activity of fibronectin can be duplicated
by small synthetic fragments of the molecule. Nature 1984;309:30
–
3.
[14]
Taubenberger V, Woodruff MA, Bai H, Muller DJ, Hutmacher DW. The effect of unlocking
RGD-motifs in collagen I on pre-osteoblast adhesion and differentiation. Biomaterials
2010;31:2827
–
35.
[15]
Leung KS, Siu WS, Cheung NM, Lui PY, Chow DH, James A, Qin L. Goats as an osteopenic
animal model. J Bone Miner Res 2001;16:2348
–
55.
[16]
Leung KS, SiuWS, Li SF, Qin L, Cheung WH, Tam KF, Lui PP. An in vitro optimized injectable
calcium phosphate cement for augmenting screw fixation in osteopenic goats. J Biomed
Mater Res B Appl Biomater 2006;78:153
–
60.
[17]
Siu WS, Qin L, Cheung WH, Leung KS. A study of trabecular bones in ovariectomized goats
with micro-computed tomography and peripheral quantitative computed tomography.
Bone 2004;35:21
–
6.
[18]
Tam KF, Cheung WH, Lee KM, Qin L, Leung KS. Shockwave exerts osteogenic effect on
osteoporotic bone in an ovariectomized goat model. Ultrasound Med Biol 2009;35:1109
–
18.
[19]
Donath K, Breuer G. A method for the study of undecalcified bones and teeth with
attached soft tissue. J Oral Pathol 1982;11:318
–
26.
[20]
Constantz BR, Ison IC, Fulmer MT, Poser RD, Smith ST, VanWagoner M, et al. Skeletal
repair by in situ formation of the mineral phase of bone. Science 1995;267:1796
–
9.
[21]
Alt V, Thormann U, Ray S, Zahner D, Dürselen L, Lips K, et al. A new metaphyseal bone
defect model in osteoporotic rats to study biomaterials for the enhancement of bone
healing in osteoporotic fractures. Acta Biomater 2013;9:7035
–
42.
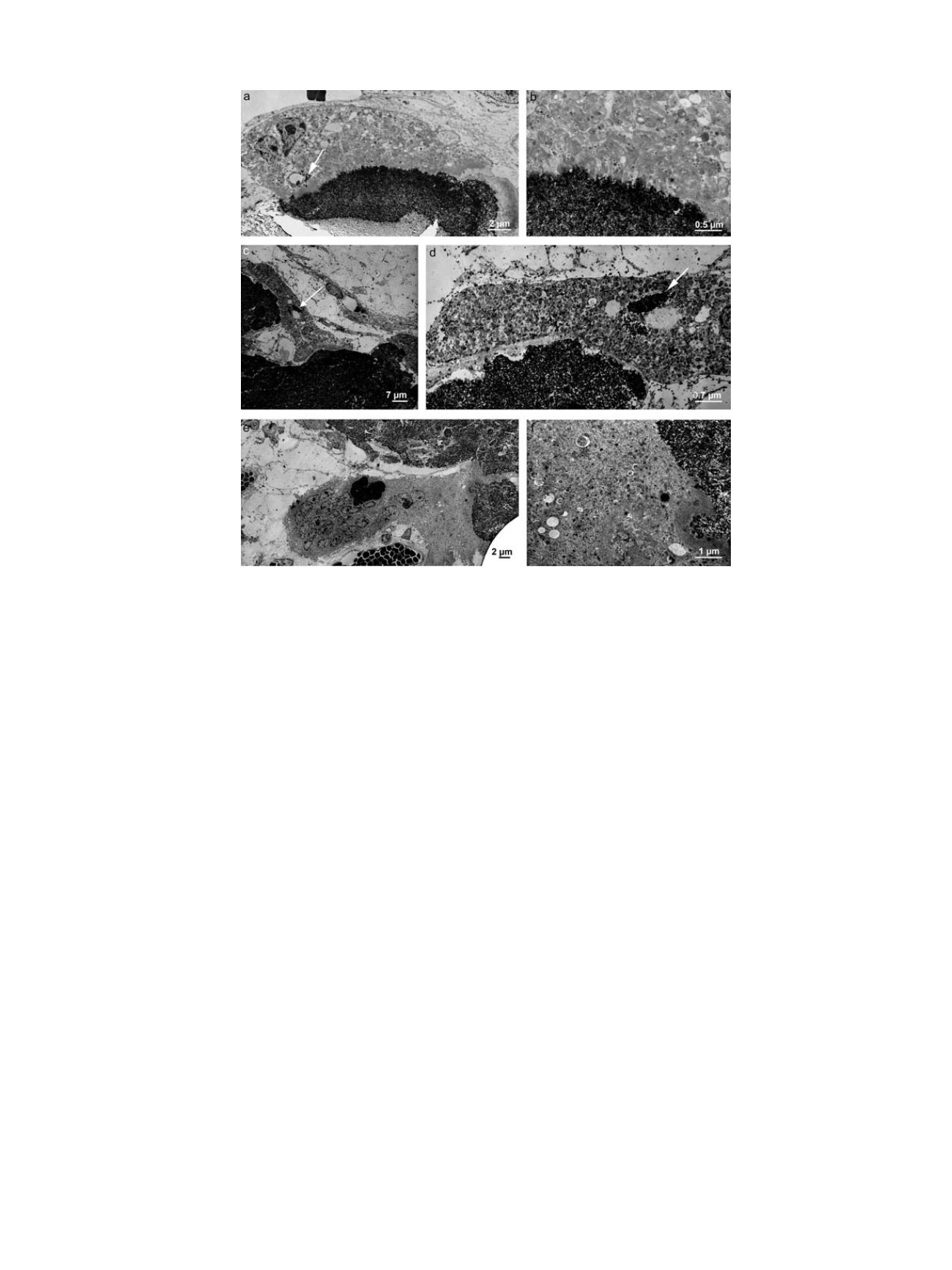
Fig. 5.
Transmission electron microscopy. Osteoclast-like cell localized in vicinity to a HA fragment with intracellular uptake of HA fragments (arrow) (
a
) and formation of a
ruffled border like resorption zone (
b
). Intracellular accumulation of HA remnants (arrows) by an osteoclast-like cell in vicinity to a HA fragment at lower (
c
) and higher magnifi-
cation with distribution of implant remnants within the entire cytoplasm (
d
). Osteoclast-like cell in the vicinity to a HA/col-1 implant with a high number of nuclei (
e
) and only
a small contact zone without formation of a ruffled border (
f
).
V. Alt et al. / Injury, Int. J. Care Injured 47S2 (2016) S58
–
S65
S65


















