
Management principles of osteoporotic fractures
Michael J. Gardner, Cory Collinge*
Vanderbilt University Medical Center, Medical Center East- South Tower, Nashville, TN 37205, United States
A B S T R A C T
Osteoporotic fractures are difficult to manage. They pose a number of difficulties to the surgeon arising from the
underlying poor bone stock compromising the intention to achieve optimum fixation. Moreover, the frail elderly
patients present with a variety of medical co-morbidities increasing the risk of developing perioperative
complications. Despite these recognized challenges, there are currently a number of improving technologies and
strategies at the surgeon
’
s disposal to provide more confidence with fracture fixation and maximize the chance of
success.
© 2016 Elsevier Ltd. All rights reserved.
K E Y W O R D S
Fixation
Osteoporotic fractures
Locked plating
Augmentation
Challenges in the treatment of osteoporotic fractures
Over the next several decades, the increasing number of patients
expected to experience osteoporotic fractures, the so-called
“
silver
tsunami,
”
is already being sensed by orthopaedic surgeons and others
who provide care to elderly patients. These patients are characterized
by physical frailty, medical co-morbidities, and general immobility.
When fractures occur in these patients, fixation often rendered
unpredictable by the poor holding power of internal fixation within
osteoporotic bone [1]. These situations are also made more complex by
their periarticular, periprosthetic, or even interprosthetic fracture
locations [2,3]. The repair of these fractures require a thoughtful, and
often unique, approach to maximize the strength of repair to allow
patients to mobilize as soon as is feasible. Despite these recognized
challenges, there are currently a number of improving technologies
and strategies at the surgeon
’
s disposal to provide more confidence
with fracture fixation and maximize the chance of success.
Locked plating
One component of the pathological process in osteoporosis involves
cortical thinning, which is often magnified in the metaphyseal or
metadiaphyseal regions of long bones. Hence, osteoporotic fractures
often occur in these regions. When these occur, the articular, or
epiphyseal, fracture segment is often relatively small, making fixation
with intramedullary nail interlocking screws problematic. Thus,
plating of these fractures has historically been the technique of
choice. With standard plating constructs, plating on one surface of a
metaphyseal fracture (eccentric stabilization) can be particularly prone
to fixation failure [4]. Mechanically, the ability of the screw head
to toggle within the plate make it difficult for these implants to
maintain coronal plane alignment, particularly with opposite-cortex
comminution [5,6]. Because most plates are applied laterally, medial
cortical comminution predisposes to reduction loss with varus
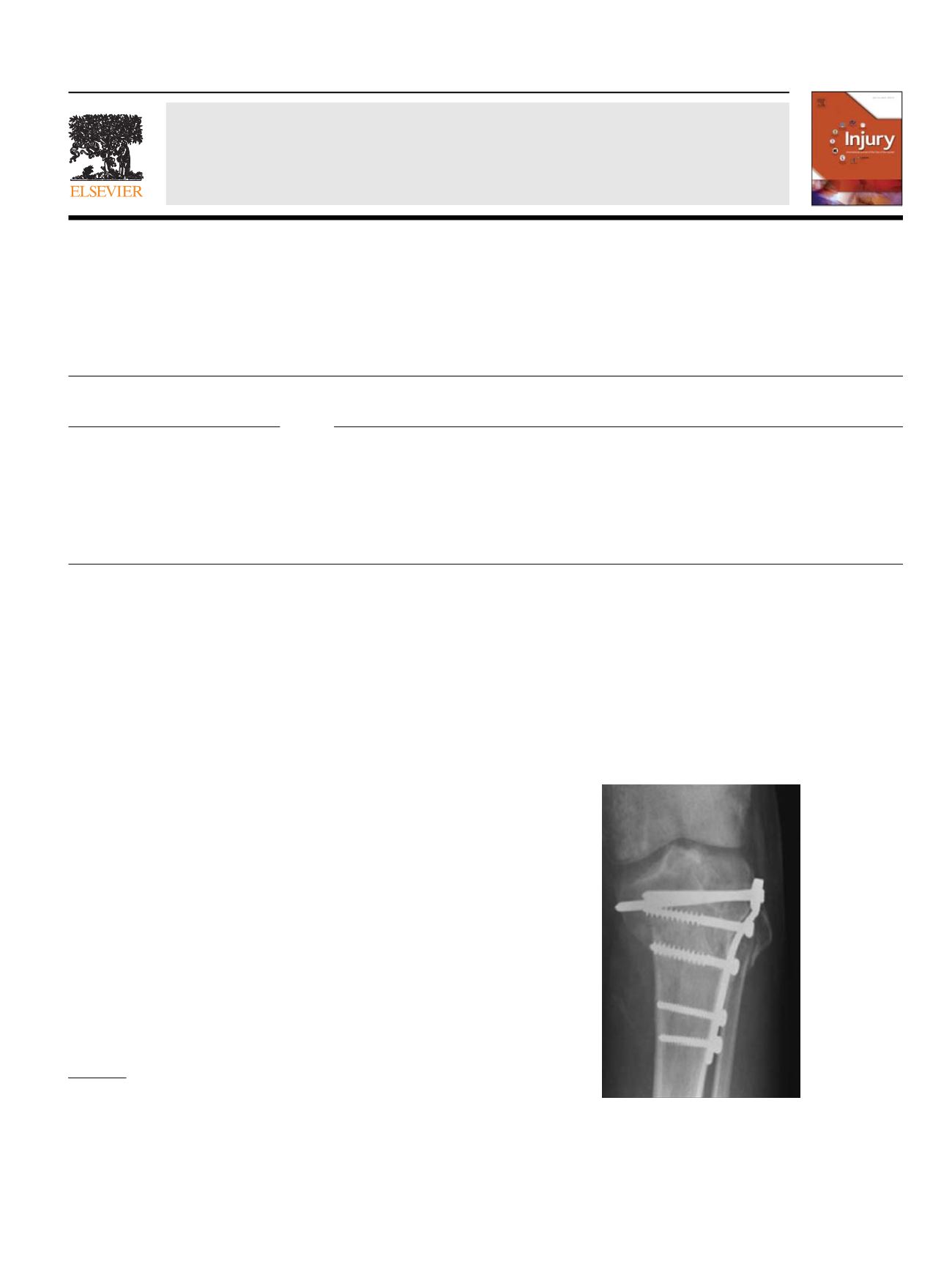
deformity when standard implants are used (Figure 1).
Fig. 1.
Example of a proximal tibial metaphyseal treated with a lateral standard
(non-locked) implant. Varus failure occurred.
*
Corresponding author at: Cory Collinge, MD. Professor of Orthopedic Surgery, Department
of Orthopedic Surgery, Vanderbilt University Medical Center, Medical Center East- South
Tower, Suite 4200, Nashville, TN 37205. Tel.: (817) 253-9392.
E-mail address
:
ccollinge@msn.com(C. Collinge)
Injury, Int. J. Care Injured 47S2 (2016) S33
–
S35
Contents lists available at ScienceDirect
Injury
journal homepage: www.
elsevier.com/locate/Injury0020-1383 / © 2016 Elsevier Ltd. All rights reserved.


















